THE VALUE OF VIRTUAL HUMANS: THEY'RE BETTER THAN REAL PEOPLE
10 QUESTIONS TO BOOST YOUR UNDERSTANDING OF VIRTUAL HUMANS' BENEFIT IN TEACHING COMMUNICATION SKILLS
 Experts agree. Generation Z has abysmal communication skills.
Experts agree. Generation Z has abysmal communication skills.It makes sense, of course. Gen Z students have had little opportunity to hone interpersonal skills. For their entire lives, most of their communication with others has taken place through technology, rather than in person. (Consider that "the only communication methods that Generation Z has known include buttons to send messages, mailboxes that cannot be physically touched, and photo albums that are stored in a cloud," write the authors of Generation Z goes to college.)
This lack of interpersonal communication skills puts nursing students at a considerable disadvantage. And their opportunities for developing these skills has already been on a decline. For years now, nursing students have had fewer opportunities to work in clinical settings (the pandemic certainly hasn't helped) and, thus, have had challenges developing the therapeutic skills necessary for conversing successfully with clients — especially high-risk clients. Now, that inexperience is coupled with a lack of inherent communication skills due to growing up in a world where technology has filled that role.
The result? Students and new nurses feel vulnerable and insecure when suddenly faced with critical conversations.
Several years ago, recognizing the existing need for these vital skills and anticipating that the problem was getting worse, the Product Management Team at ATI began researching best practices on how to successfully connect with and educate students. They wanted a solution that would focus particularly on building students’ confidence in talking with diverse and high-risk clients.
The team determined that creating a realistic, simulated experience in which students could practice for as long as necessary would be the most impactful — and cost-effective.
We interviewed Mark Williams-Abrams, ATI Vice President of Product Strategy, to get some details on what the Product Team has developed.
DOWNLOAD THE INFOGRAPHIC AT RIGHT AS A HANDY REFERENCE
Question 1: What’s changed in students’ lives that’s caused them to need help in developing better communication skills?
MWA: Most experts point to the digital age we live in — with its much greater use of text messages and social media. Because that technology is such a huge part of today’s students’ lives, they haven’t needed to develop the types of communication skills — especially therapeutic communication skills — that nurses in particular require. But we know those skills play a critical role in students’ ability to identify unhealthy client behaviors and motivate them to make changes that could save their lives.Q2: What did the Product Management Team’s studies uncover in helping to solve this problem?
 MWA: Our team looked at the most recent developments in technology and research. We already knew there’s a lot of new and unique ways to teach people how to effectively lead conversations, but we were especially interested in techniques that can measurably improve social, emotional, and physical health.
MWA: Our team looked at the most recent developments in technology and research. We already knew there’s a lot of new and unique ways to teach people how to effectively lead conversations, but we were especially interested in techniques that can measurably improve social, emotional, and physical health. We took a deep dive into the latest information on virtual humans, simulations, and social cognitive communication strategies, and we also looked at the increasing adoption of online instructional technologies within health and behavioral health.
That research led us to pursue multiple new solutions using virtual humans and an online platform. A lot of research supports the success of this type of simulation-focused learning.
Q3: What was one of the first solutions your team developed?
MWA: A few years ago, we added a new component to our Nurse’s Touch series. We refer to it as The Communicator 2.0. Basically, what we’ve created is a tool that guides students through therapeutic communication techniques and gives them repeated opportunities to engage in key client conversations. We were especially focused on those conversations students need to have with high-risk clients. We wanted to help them learn and practice communication techniques that really make a difference and drive change in client behavior.
Up until now, Nurse’s Touch was made up of interactive, video-based product features. Our goal with The Communicator 2.0 was to raise the bar with how we bring educational scenarios to our users.
Virtual interactions immerse students in situations with clients portrayed by virtual humans. The students learn, practice, and apply therapeutic communication skills in a safe, virtual, simulated clinical environment.
Today, we're continuously developing new simulations that feature virtual humans. In addition to The Communicator 2.0, we also offer:
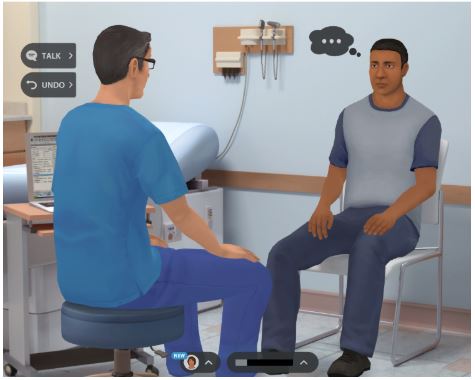 Q4: Describe what makes virtual humans impactful. After all, they’re not real. How can they provide deeper learning than working with a real human?
Q4: Describe what makes virtual humans impactful. After all, they’re not real. How can they provide deeper learning than working with a real human?
MWA: Basically, it’s the fact that they are virtual and not real-life people. That may seem counter-intuitive, because you may assume that no one can teach one human how to communicate better than another human. But research shows that’s not the case. After all, consider being a student and trying to learn and practice in front of peers or faculty. Who wants to make a mistake in front of their peers and teacher? And you certainly don’t want to begin your practice on real clients and say or do something wrong that puts clients at risk.So there’s a huge intimidation factor that makes role-playing with real humans less effective than teaching with virtual humans. They completely remove that factor and present students with a practice environment that feels comfortable and safe for exploring and learning.
Q5: But aren’t virtual humans just, like, cartoons of people?
MWA: Not at all. And that’s where the technology makes such a difference. Today’s advancements allow us to create incredibly effective realism that’s totally believable. The virtual humans who are part of our new solutions have been designed to mimic human behavior in terms of appearance, emotional responses, body language, facial expressions, and tone of voice.You can’t really appreciate their level of realism until you interact with them.
But we’ve also learned that virtual humans can’t be too realistic. Research shows that learning, retention, and engagement are actually undermined by overly realistic characters. So we’ve taken that information into account in developing our virtual humans.
Q6: What other aspects of virtual humans should educators understand to appreciate their value?
MWA: The safety factor is especially important. Practicing in a virtual environment is obviously safer because you can’t make a mistake that will endanger a patient’s life.Interactions in this virtual world also build students’ confidence as they practice new techniques over and over. When it’s time to work with a real client, the student feels very prepared.
Another advantage is that every students’ experience is the same in the virtual world. You’ll never have to worry about peer actors in live simulations not taking their roles seriously or deviating from the plan and negatively impacting other students’ learning.
Q7: That consistency seems like it would be a real advantage to educators, as well as students. What are the other advantages to educators?
 MWA: Using a virtual solution alleviates a lot of time and workload stressors for faculty. For one, students always have access to the virtual simulations — 24/7 — from any computer with an internet connection. So that relieves a lot of an educator’s time.
MWA: Using a virtual solution alleviates a lot of time and workload stressors for faculty. For one, students always have access to the virtual simulations — 24/7 — from any computer with an internet connection. So that relieves a lot of an educator’s time.Along those same lines, instructors don’t need to schedule lab time, because students work on their own. And they don’t have to develop cases or coordinate with colleagues to create simulation activities.
Third, our simulations bring a level of ease to the evaluation process that educators will really appreciate, as well as that consistency I mentioned previously; all students have the exact same experiences.
Q8: What else about virtual simulation do you prefer over options like video?
MWA: Video can be extremely, extremely effective. But one advantage virtual humans have over actors or real-life healthcare workers is that they “age” better than video. Styles, settings, equipment, and practice change over time. All of these aspects can be costly to maintain and remain consistent. Virtual humans don’t age!Q9: What are the best ways for educators to use virtual simulations?
MWA: The opportunities are, honestly, endless. You can incorporate virtual activities into the classroom or the lab, or you can assign them as homework or clinical prep. Or you can develop small-group and large-group activities with debriefings. It’s really up to the educators’ creativity.Our lesson plans for products featuring virtual humans make it seamless for faculty to incorporate them into these simulations into their curricula. That means students are better prepared for clinicals and professional practice.
Q10: What specific topics does Nurse’s Touch, The Communicator 2.0, address?
MWA: We focused on developing modules that help students develop communication skills in areas that are most common — and also that can be the most uncomfortable to talk about. In today’s world, those topics include:
- clients and their nutritional needs
- adolescent clients and performance-enhancement substances
- adult clients misusing alcohol
- adolescent clients at risk for suicide
- adult clients at risk for medication misuse and suicide.
We’ve discovered that a lot of users often spend more time in the simulation than required. A lot of them decide to play more than once. When we asked them about it, they said they were curious about different reactions and wanted to explore different approaches. Some wanted to see what happened when they instigated negative responses. And a lot said they were simply having fun.
You can’t beat a tool that teaches and entertains. That’s the best solution yet.
RESOURCES
- Seemiller, C., & Grace, M. (2016). Generation Z goes to college. San Francisco: Jossey-Bass.
